Mohammad Amin Keikhanejad1*, Mahdie Keikhanejad2
1 Zahedan University of Medical Sciences, Zahedan, IR Iran
2 Iran University of Medical Sciences, Tehran, IR Iran
* aminkeikhanejad@zaums.ac.ir
Abstract
Transgender individuals face significant global mental health disparities, largely driven by discrimination, stigma and limited access to care. These challenges are particularly severe in Iran, where cultural, legal and societal barriers intensify psychological stress. This study aimed to synthesize existing research on the mental health state among transgender people in Iran, including key insights, research gaps and future research regarding intervention research directions. A systematic search of PubMed, Google Scholar and Science Direct identified studies published since 2014. Inclusion required alignment with DSM-5 definitions and the use of standardized mental health instruments. This study assessed methodological quality using the Newcastle–Ottawa Scale and the Critical Appraisal Skills Program. The reviewed studies consistently reported high prevalence of depression, anxiety and suicidal ideation. Additional findings included obsessive–compulsive disorder, somatization, substance use disorders and psychotic symptoms. Stigmatization, restrictive legal frameworks and limited access to gender-affirming care were major contributing factors. Evidence suggests gender-affirming interventions improve outcomes, though access in Iran remains extremely limited. Existing studies, often cross-sectional with small samples, limit generalizability. Future research should prioritize longitudinal designs, larger and more diverse samples and intervention-based studies to better inform policy and practice.
Introduction
The term ‘transgender’ has evolved since its early usage in the 1960s, when it described individuals living in a gender role different from their assigned sex (Feinberg 1992; Hill 2007; Stryker 2008). Today, according to the American Psychological Association (APA), 'transgender' is a broad classification for individuals whose gender identity, expression or behavior does not align with the sex stereotypes typically assigned to them at birth. (American Psychological Association 2023) Despite the growing recognition of transgender identities, many transgender people still endure significant barriers, particularly with regard to mental health, which are largely driven by societal stigma, discrimination and stressors tied to their gender nonconformity. (Pinna et al. 2022; Strauss et al. 2020)
While some social perspectives have historically misunderstood transgender identities as inherently linked to mental disorders, understanding the historical context clarifies that transgender individuals face unique vulnerabilities—especially regarding mental health—that stem largely from external social factors rather than their gender identity itself. According to the American Psychological Association (APA), a mental disorder is defined as a psychological condition that causes significant distress or impairment in daily functioning. Most transgender individuals do not find their gender identity distressing or disabling, meaning that being transgender in itself does not constitute a mental disorder. (American Psychological Association 2023) However, transgender individuals, particularly youth, face disproportionately high rates of mental health issues, such as depression, anxiety and suicidal ideation, often stemming from discrimination, bullying and peer rejection (Pinna et al. 2022). One prominent example highlighting these mental health challenges is a retrospective 2015 cohort study led by Sari L. Reisner. This study found that transgender youth are at a significantly higher risk of being diagnosed with DSM-IV-TR depression (50.6% vs. 20.6%), anxiety (26.7% vs. 10.0%), suicidal ideation (31.1% vs. 11.1%), suicide attempts (17.2% vs. 6.1%) and non-lethal self-harm (16.7% vs. 4.4%) compared to cisgender matched peers (Reisner et al. 2015). These findings underscore mental health issues as one of the most critical aspects of transgender individuals' lives, as they face disproportionately higher rates of depression, anxiety, suicidal ideation and self-harm.
While global research demonstrates elevated rates of depression, anxiety and suicidality among transgender populations, these risks are compounded in Iran by unique structural and cultural stressors, making focused research in this context especially urgent. The realities of sexual and gender minorities in Iran have long been shaped by legal and cultural barriers. In February and March of that year, sixteen individuals were executed for crimes related to sexual violations (Whitaker 2007). Despite facing significant legal barriers, LGBTQ+ individuals in Iran also grapple with pervasive cultural challenges, such as stigma and discrimination. These harsh societal conditions create a uniquely difficult environment, particularly for transgender individuals. Understanding the specific mental health issues faced by this community becomes even more crucial considering the epidemiological data (Amnesty International 2022; Human Rights Watch 2010; U.S. Institute of Peace [The Iran Primer] 2024). Based on a 2017 statistical report examining the prevalence of gender dysphoria among individuals over the age of 18 in Iran, the overall prevalence was found to be 1.46 per 100,000 individuals of the general population. Specifically, the prevalence of transgender men (assigned female at birth) was 0.94 per 100,000 while the prevalence of transgender women (assigned male at birth) was 2.00 per 100,000 (Statistical Center of Iran 2017; Talaei et al. 2022).
Taken together, these findings highlight the urgent need to better understand the mental health challenges of transgender individuals in Iran. Although several studies have explored these issues in specific cities, no prior synthesis has systematically examined the evidence, evaluated methodological rigor and identified research gaps. The aim of this narrative review is therefore to consolidate existing research on the mental health of Iranian transgender people, critically assess its quality and highlight future directions for research and interventions. By situating the Iranian experience within the global literature, this review underscores the distinct challenges created by the intersection of stigma, legal restrictions, limited access to care and contributes new insights to guide policy and clinical practice.
Methods
This narrative review aims to synthesize the current evidence on the mental health of transgender individuals in Iran. A literature search was performed using PubMed, Google Scholar and ScienceDirect. The search strategy combined keywords such as “transgender,” “mental health,” and “Iran,” and was limited to articles published in the last 10 years (2014 onward) to ensure relevance to contemporary social and legal contexts in Iran. Studies were eligible for inclusion if they were published in English, based on the DSM-5 definition of transgender identities to avoid derogatory terminology, and employed either cross-sectional designs or qualitative interviews providing direct insights into the experiences of transgender individuals. Studies relying on DSM-IV definitions or using offensive or outdated terminology were excluded.
After applying these criteria, the review included a total of 11 studies. The selected studies captured a range of methodological approaches, geographic regions within Iran and participant demographics, providing a comprehensive overview of available research. Quality assessment of the selected studies was conducted using the Newcastle-Ottawa Scale (NOS) for cross-sectional studies and the Critical Appraisal Skills Programme (CASP) for qualitative research. NOS assesses three domains ,selection, comparability and outcome, to determine study quality, while CASP evaluates rigor, credibility and relevance in qualitative research (Critical Appraisal Skills Programme 2018; Wells et al. 2000). Two reviewers independently screened all identified articles and assessed their quality, resolving discrepancies through discussion and consensus. This approach ensured that only studies meeting minimum methodological standards were synthesized.
Results
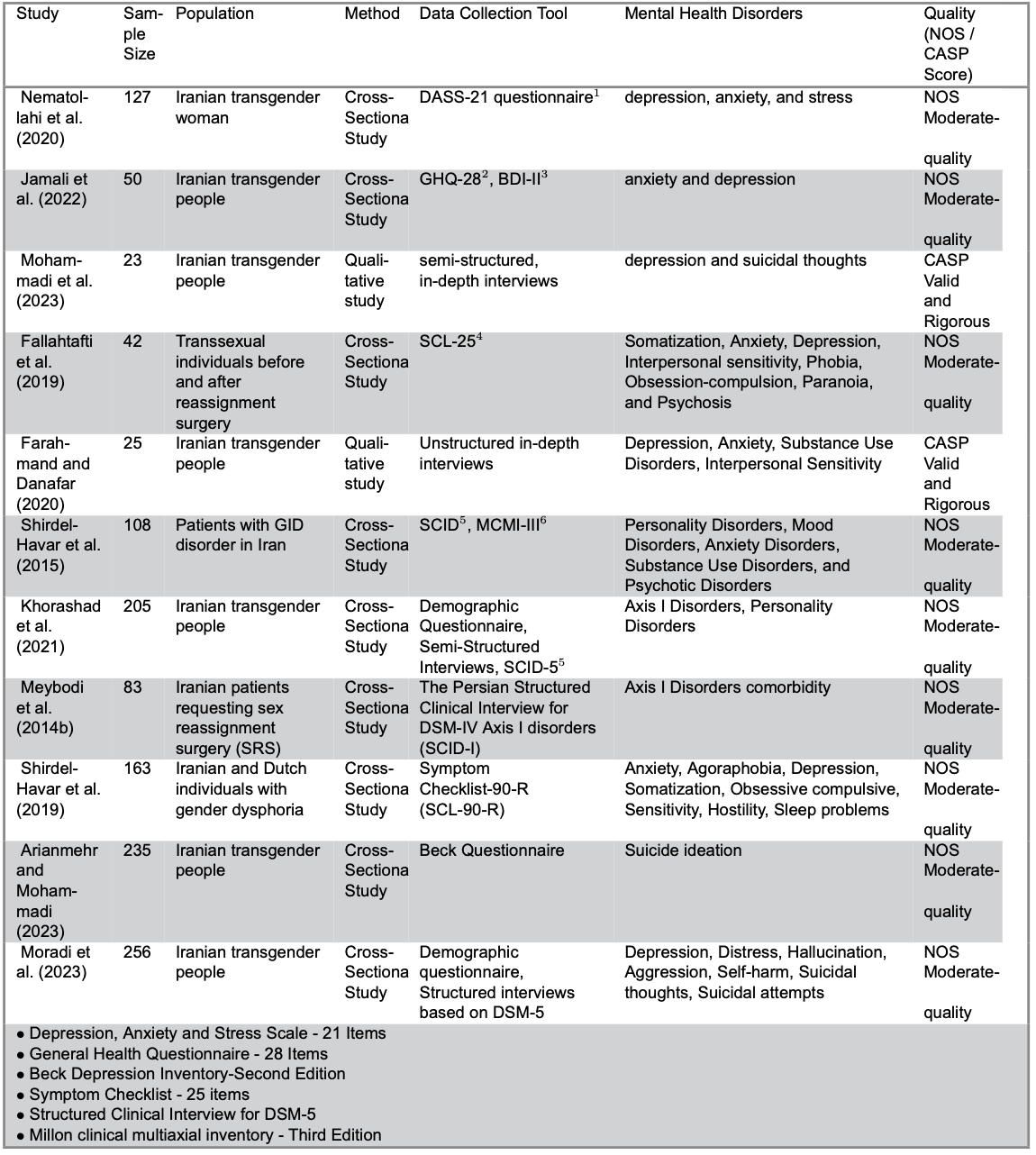
Eleven studies (total N = 1,317; Table 1) met the inclusion criteria. 10 of the 11 studies documented consistent reports of depression and anxiety. For example, Nematollahi et al. (2020) (n = 127) and Jamali et al. (2022) (n = 50) reported elevated rates of both conditions using validated screening tools (DASS-21, GHQ-28 and BDI-II). Suicidal ideation and attempts were also highly prevalent. Arianmehr et al. (2019) (n = 235) found suicidal ideation to be one of the most frequent mental health concerns, while Moradi et al. (2023) (n = 256) documented suicidal thoughts, self-harm and suicide attempts.
Other disorders included somatization, obsessive–compulsive disorder (OCD), paranoia, interpersonal sensitivity, psychosis and substance use disorders, as reported in studies such as Fallahtafti et al. (2019) (n = 42) and Shirdel-Havar et al. (2015; 2019) (n = 108, 163). Sleep problems and hostility were also noted. Axis I comorbidities were common, and two studies additionally reported personality and mood disorders. (Mazaheri Meybodi et al. 2014; Khorashad et al. 2021)
Methodological appraisal indicated that most cross-sectional studies were of moderate quality according to NOS, while the two qualitative studies (Mohammadi et al. 2023; Farahmand and Danafar 2020) were rated as valid and rigorous using CASP.
Table 1. Consolidated studies of mental health in Iran.
Discussion
Summary of Key Findings
This review synthesized 11 studies (N = 1,317) and found consistently high rates of depression, anxiety and suicidal ideation among Iranian transgender individuals, with additional reports of post-traumatic stress disorder (PTSD), OCD, somatization and substance use disorders. The reviewed studies reveal a worrying picture of mental health among transgender individuals in Iran. High prevalence rates of significant mental health disorders, such as anxiety, depression and (PTSD) have been consistently reported. Other frequently identified conditions include somatization, interpersonal sensitivity, phobia, OCD, paranoia, psychosis, substance use disorders and various personality and mood disorders.
Alarmingly, proportions of suicidal ideation and self-harm are remarkably high, emphasizing the urgent need for targeted mental health interventions. The contributing factors to these mental health challenges encompass societal stigma, discrimination, legal barriers and limited access to appropriate healthcare services. Despite the severe mental health issues faced by the Iranian transgender population, there is a lack of comprehensive mental health services and support systems tailored to their unique needs.
The mental health of transgender individuals in Iran is characterized by high rates of mental health disorders and comorbidities, highlighting the pressing need for targeted interventions and supportive policies.
Depression
Based on the review of cross-sectional studies that assessed the mental health status of the transgender community using validated questionnaires (The Persian Structured Clinical Interview for DSM-IV Axis I disorders [SCID-I], Symptom Checklist-90-R [SCL-90-R], Beck Questionnaire, Millon Clinical Multiaxial Inventory–III (MCMI-III) and Sociodemographic Questionnaire), depressive disorders are the most prevalent mood disorders among transgender individuals (Meybodi et al. 2014; Shirdel-Havar et al. 2015; Khorashad et al. 2021; Moradi et al. 2023). Nematollahi et al. (2020) reported that 22% of the target population suffers from moderate to severe depression and found an inverse relationship between the quality-of-life index and depression. According to Jamali et al. (2022), there is no significant difference in mental health indicators between Iranian transgender individuals residing in Iran and those living in Germany. Mohammadi et al. (2023) argued that factors such as lack of acceptance by society and family, negative perceptions, inappropriate behavior and language, social stigma, absence of awareness campaigns and the incongruence between mind and body contribute to the increased likelihood of mood disorders, including depression, among transgender individuals (Mohammadi et al. 2023). Farahmand and Danafar (2020) asserted that negative judgment, labeling, discrimination and rejection by family, friends and society exacerbate mental health issues in transgender individuals. The absence of a supportive system, social marginalization and deprivation further contribute to increased psychological distress (Farahmand and Danafar 2020). Fathollahi et al. (2019) highlighted that gender-affirming surgeries can enhance life satisfaction and reduce mental health problems, including depression.
A recurring theme is the negative impact of social exclusion, lack of support and the absence of awareness campaigns, which reinforce the link between external stressors and increased depression (Farahmand and Danafar 2020; Nematollahi et al. 2020). Additionally, while most studies focus on the adverse mental health outcomes of transgender individuals living in different countries, Jamali et al. (2022) offer a differing perspective by reporting no significant difference in mental health indicators between Iranian transgender individuals residing in Iran and those living in Germany. This challenges the assumption that geographic location alone significantly alters mental health outcomes, as well as the notion that community culture has a major effect, regardless of the country of residence (Jamali et al. 2022). These findings highlight the multifaceted nature of depression in transgender individuals, shaped by both social adversity and the potential benefits of medical transition.
The findings of these studies, which highlight elevated levels of depression among Iranian transgender individuals, are consistent with international data. For instance, a large-scale study by Hajek et al. (2023) reported that transgender individuals experience disproportionately higher rates of mental health disorders, including major depressive disorder and generalized anxiety disorder, compared to their cisgender counterparts.
Anxiety
According to the studies by Farahmand et al. (2020) and Khorashad et al. (2021), anxiety is not only recognized as an independent risk factor within the transgender community but also acts as an exacerbating factor for depression. The presence of anxiety and stress, experiences of failure, dissatisfaction with oneself, life and society, as well as a lack of self-confidence, can contribute to the worsening of depressive symptoms. Furthermore, Farahmand and Danafar (2020) suggest that transgender individuals, due to the experience of identity duality and the inability to answer questions regarding their gender identity, may be more susceptible to anxiety and depression.
In a cross-sectional study by Mazaheri Meybodi et al. (2014), it was found that 36% of the target population suffered from an anxiety disorder, while 6% experienced generalized anxiety disorder. Shirdel-Havar et al. (2019) argued that the misidentification of transgender individuals with homosexual individuals leads to discrimination against them. This misperception can result in a lack of support from family and friends, as well as arrests by the police and other law enforcement agencies. Although these incidents may not cause direct physical harm, they can lead to severe internal and psychological conflicts, including anxiety and depression (Shirdel-Havar et al. 2019).
Nematollahi et al. (2020), through an analysis of quality-of-life indices, identified a significant inverse relationship between anxiety and quality of life. They reported that 20% of the target population experienced severe or moderately severe anxiety. Their findings indicate that for each level of educational attainment, there is a corresponding 6% reduction in anxiety and an 8% decrease in stress levels. Additionally, Shirdel-Havar et al. (2019) highlight that, as expected, the prevalence of anxiety and other psychological disorders among Iranian transgender individuals is higher compared to their Dutch counterparts (Shirdel-Havar et al. 2019).
Moradi et al. (2023) asserted that low self-esteem and poor interpersonal functioning are key predictors of anxiety. Moradi et al. (2023) and Fathollahi et al. (2019) considered hormone therapy and gender-affirming surgery as effective interventions for reducing anxiety.
Studies on anxiety in the transgender community consistently emphasize its role as both an independent risk factor and an exacerbating factor for depression, with common themes highlighting the psychological distress stemming from identity struggles, societal rejection and lack of self-confidence (Farahmand and Danafar 2020; Khorashad et al. 2021). Additionally, Nematollahi et al. (2020) found that higher education levels correlate with reduced anxiety, suggesting that socioeconomic factors may serve as protective influences. These findings underline the multifaceted nature of anxiety in transgender individuals, shaped by a complex interaction of personal, social and medical factors.
The studies’ findings are supported by international research. Bouman et al. (2017) have similarly identified low self-esteem and interpersonal functioning as key psychological and social factors contributing to heightened anxiety in transgender populations. This alignment reinforces the broader understanding that transgender individuals face unique stressors that significantly impact their mental health across different cultural settings.
Suicidal Ideation and Self-Harm
The statistics related to suicide within the Iranian transgender community are deeply concerning. Khorashad et al. (2021) reported these alarming figures in their study: among the target population, 18.5% had engaged in self-harm, 19% had attempted suicide and 50% had experienced suicidal ideation. Similarly, Javaheri et al. (2010) stated that as a result of rejection by both family and society, 65% of the target population had contemplated suicide. Moradi et al. (2023) further reported that the prevalence of suicidal ideation, self-harm and suicide attempts in their study was 52.2%, 39.9% and 33.9%, respectively.
Farahmand and Danafar (2020) argued that the psychological distress and numerous societal restrictions imposed on transgender individuals are sufficient to drive them toward suicidal behavior. Additionally, they highlight that gender-related conflicts play a significant role in self-harm, suicidal thoughts and even suicide attempts.
Arianmehr et al. (2019) discussed the impact of familial factors, such as neglect, ridicule, enforced traditional gender clothes and physical abuse, as major contributors to suicidal ideation among transgender individuals. They also noted a decline in suicidal ideation with aging (Arianmehr and Mohammadi 2023). Although Arianmehr et al. (2019) did not identify a significant correlation between education level and suicidal thoughts in their study, they reference other research suggesting a potential association between higher education levels and increased suicidal ideation (Asadipour et al. 2019).
Moradi et al. (2023) identify suicidal ideation and suicide attempts as the most prevalent psychological issues among transgender individuals, second only to depression. Their findings indicate that the prevalence of self-harm and suicide attempts is higher among married transgender individuals. Additionally, Moradi et al. (2023) suggests that transgender individuals with independent employment and income are at a higher risk of suicide than those receiving financial support from their families. Furthermore, they reported that transgender individuals engaged in sex work experience suicidal ideation at a rate seven times higher and suicide attempts at a rate 11 times higher than other members of the transgender community.
Finally, Arianmehr and Mohammadi (2023) highlighted that transgender individuals who undergo medical treatments, such as hormone therapy and gender-affirming surgery, show a reduction in both suicidal ideation and suicide attempts.
The theme of suicidal ideation and self-harm among transgender individuals consistently emerges across studies, with societal rejection, psychological distress and gender-related conflicts identified as key contributors to these behaviors (Farahmand and Danafar 2020; Khorashad et al. 2021; Moradi et al. 2023). A recurrent finding is the high prevalence of suicidal ideation, self-harm and suicide attempts, which are often intensified by familial neglect, ridicule and societal restrictions (Arianmehr and Mohammadi 2023). However, contrasting findings arise regarding the impact of factors like education, employment and sex work. While Arianmehr et al. (2023) reported no significant correlation between education level and suicidal thoughts, Moradi et al. (2023) highlighted that transgender individuals with higher education and independent employment are at greater risk of suicide, suggesting a complex relationship between socioeconomic factors and suicidal ideation. These findings underscore the multifaceted nature of suicidal ideation and self-harm in transgender individuals, shaped by both social and medical factors.
The findings of this study, which show that gender nonconforming transgender individuals face higher levels of discrimination and engage more in health-harming behaviors, including suicide attempts, align with international research. Studies like Miller and Grollman (2015) have similarly demonstrated that transgender individuals—particularly those who are gender nonconforming—are at significantly higher risk for suicide attempts compared to the general population. This highlights the critical role of societal stigma and discrimination in exacerbating mental health challenges within the transgender community, reinforcing the need for targeted interventions.
Other Mental Health Disorders
Khorashad et al. (2021) reported that 67.3% of the target population had experienced one or more Axis I disorders during their lifetime. These disorders included trauma- and stressor-related disorders, obsessive-compulsive disorder (OCD), substance use disorders and addiction, bipolar disorder, schizophrenia and neurocognitive disorders.
Similarly, Mazaheri Meybodi et al. (2014) indicated that 62.7% of the target population had been diagnosed with Axis I disorders throughout their lifetime. The most prevalent disorders in this group were specific phobia (20.5%), adjustment disorder (15.7%), substance use disorder (8.4%), dysthymic disorder (7.2%), OCD (6%) and finally, social phobia, panic disorder and alcohol abuse, each with a prevalence of 4.8%.
Shirdel-Havar et al. (2019), utilizing the Symptom Checklist (SCL), identified the most common disorders in the following order: anxiety, somatization, depression, OCD, sleep disturbances and interpersonal sensitivity. Additionally, Shirdel-Havar et al. (2015) examined Axis I disorders based on the DSM criteria and reported the most prevalent disorders as follows: post-traumatic stress disorder (PTSD) (15.7%), major depressive disorder (13.9%), specific phobia (11.1%) and body dysmorphic disorder (10.2%).
Moradi et al. (2023) reported that 15.5% of the target population had experienced hallucinations at some point in their lives. Furthermore, Fathollahi et al. (2019), in a study examining patients before and after surgery, found a significant post-surgical reduction in somatization, interpersonal sensitivity, phobias, OCD, paranoia and psychosis within the target population.
The studies collectively highlight the high prevalence of various Axis I disorders among transgender individuals, with trauma and stressor-related disorders, OCD, substance use disorders and mood disorders like depression and anxiety emerging as consistent themes (Khorashad et al. 2021; Mazaheri Meybodi et al. 2014; Shirdel-Havar et al. 2015). These disorders are often exacerbated by societal factors such as discrimination and trauma, contributing to their persistence. These variations illustrate the complex interplay of social, psychological and medical factors in the mental health of transgender individuals.
Comparison with the Global Literature
This Iranian narrative review confirms what global research has long shown: transgender individuals, whether in Iran or elsewhere, are at heightened risk for mental health issues like depression, anxiety and suicidal ideation. For instance, the review shows that depression and anxiety are widespread among Iranian transgender people, with contributing factors such as family rejection, societal stigma and even legal restrictions playing a pivotal role. Globally, studies have consistently reported similar patterns. Transgender populations in Western contexts also face high rates of these disorders, which are often linked to discrimination and marginalization (Pinna et al. 2022).
However, there are noteworthy differences. While global research points to the benefits of legal protections, access to gender-affirming care and supportive social policies in ameliorating mental health risks, the Iranian context is complicated by stricter cultural and legal constraints. For example, some Iranian studies reported that the mental health of transgender individuals remains poor regardless of whether they live in Iran or abroad—suggesting that pervasive societal stigma may override the potential benefits of residing in a more accepting country.
Moreover, while the global literature often discusses a broad spectrum of supportive interventions, the review underscores the urgent need for mental health services that are tailored to overcome specific local barriers—legal, cultural and systemic.
In essence, both the Iranian findings and the global literature agree on the central role of external stressors in contributing to poor mental health outcomes. However, the Iranian experience is marked by additional layers of legal and cultural adversity, which may intensify these issues compared to settings where transgender individuals have greater access to supportive resources and legal protections.
These findings reinforce that while mental health disparities among transgender populations are a global issue, the Iranian context adds unique legal and cultural barriers that exacerbate already elevated risks.
Limitations and Future Directions
This review is limited by the quality and design of the studies it includes. The majority of reviewed research relied on small, non-representative samples, often recruited through convenience or snowball sampling. Most were cross-sectional, restricting the ability to draw causal inferences about mental health outcomes. In addition, there was considerable variability in the tools and diagnostic criteria used to assess mental health, ranging from structured clinical interviews to self-report questionnaires, which limits comparability across studies. The absence of control groups in most studies further makes it difficult to isolate factors specific to transgender individuals from broader societal stressors.
To address these gaps, future research should prioritize longitudinal designs with larger, more diverse samples that represent the transgender population across different regions of Iran. Standardizing mental health assessment tools and including cisgender comparison groups will improve reliability and contextual understanding. Future studies should also explore understudied domains such as substance use and psychotic symptoms, evaluate the impact of gender-affirming interventions on mental health and examine protective factors like social support and resilience. Comparative studies between Iranian transgender populations and those in other cultural contexts would further clarify the role of legal and social environments in shaping outcomes. Collaborations with trusted LGBTQ+ organizations and the use of anonymous, confidential methods may also enhance recruitment and data accuracy in restrictive settings.
This review has its own limitations. As a narrative review, it is subject to selection bias and does not provide pooled statistical estimates. Restricting the search to English-language publications may have led to the exclusion of relevant Persian-language or unpublished studies. These factors should be considered when interpreting the findings.
Conclusion
This narrative review highlights the profound mental health challenges confronting transgender individuals in Iran. Despite an initial pool of approximately 20 studies, strict inclusion criteria—emphasizing DSM-5 definitions and respectful language—ensured that only the most methodologically sound research was synthesized. The findings reveal alarmingly high rates of depression, anxiety and suicidal ideation, which are closely linked to pervasive societal stigma, discrimination and legal barriers.
The reviewed studies, though primarily cross-sectional and of moderate quality, consistently underscore the detrimental impact of external stressors and systemic neglect on the mental health of transgender individuals. This evidence calls for immediate action: targeted mental health interventions, improved access to gender-affirming care and the development of comprehensive support systems that are sensitive to the unique cultural and legal context of Iran.
Future research should adopt longitudinal designs to better capture the evolving mental health trajectories within this population and to evaluate the long-term effectiveness of intervention strategies. Moreover, larger, more representative studies are needed to further elucidate the complex interplay of social, psychological and legal factors influencing mental health outcomes.
In conclusion, addressing the mental health disparities experienced by transgender individuals in Iran is not only a clinical imperative but also a critical human rights issue. Collaborative efforts among researchers, clinicians and policymakers are essential to create an inclusive environment that fosters resilience and improves the overall well-being of this marginalized community.
Declaration of generative AI and AI-assisted technologies in the writing process
During the preparation of this work, the authors used ChatGPT 4o in order to improve language and readability, with caution. After using this tool/service, the authors reviewed and edited the content as needed and took full responsibility for the content of the publication.
Compliance with Ethical Standards
Funding: The authors did not receive support from any organization for the submitted work.
Conflict of Interest: The authors declare no conflicts of interest.
Ethical Approval: This article does not contain any studies with human participants or animals performed by any of the authors.
Informed Consent: Not applicable.
Data Availability: No datasets were generated or analyzed during the current study.
References
Afrasiabi, H. and Junbakhsh, M. (2019) ‘Meanings and Experiences of Being Transgender: A Qualitative Study among Transgender Youth’, The Qualitative Report. Advance online publication, available: https://doi.org/10.46743/2160-3715/2019.3594
American Psychological Association (2023) ‘Understanding transgender people, gender identity and gender expression’, available: https://www.apa.org/topics/lgbtq/transgender-people-gender-identity-gender-expression
Amnesty International (2022) Iran 2022 Human Rights Report.
Arianmehr, T. and Mohammadi, Y. (2023) ‘Suicide ideation and the related factors among Iranian transgender people: A cross-sectional study’, BMC Research Notes, 16(1), 195, available: https://doi.org/10.1186/s13104-023-06471-3
Asadipour, E., Behzadipour, S. and Zarenezhad, M. (2019) ‘Comparison of Suicidal Tendency in Male Operated and Non-operated Patients Suffering from Gender Dysphoria, in Fars Province between 2011 and 2013’, Iranian Journal of Forensic Medicine, 24(4), 31–36. ISSN: 1027-1457.
Bouman, W.P., Claes, L., Brewin, N., Crawford, J.R., Millet, N., Fernandez-Aranda, F. and Arcelus, J. (2017) ‘Transgender and anxiety: A comparative study between transgender people and the general population’, International Journal of Transgenderism, 18(1), 16–26, available: https://doi.org/10.1080/15532739.2016.1258352
Brian, W. (2007) ‘No homosexuality here’, The Guardian, available: https://www.theguardian.com/commentisfree/2007/sep/25/nohomosexualityhere
Critical Appraisal Skills Programme (2018) ‘Critical Appraisal Skills Programme Checklist’, available: https://casp-uk.net/casp-tools-checklists/
Fallahtafti, E., Nasehi, M., Rasuli, R., Farhud, D.D., Pourebrahim, T. and Zareeeimahmoodabadi, H. (2019) ‘Happiness and Mental Health in Pre-Operative and Post-Operative Transsexual People’, Iranian Journal of Public Health, 48(12), 2277–2284.
Farahmand, M. and Danafar, F. (2020) ‘Transgenders’ Mental Experiences of Gender Duality: A Qualitative Study in Iran’, Iranian Journal of Psychiatry and Behavioral Sciences, 14(2), available: https://doi.org/10.5812/ijpbs.98368
Hajek, A., König, H.-H., Buczak-Stec, E., Blessmann, M. and Grupp, K. (2023) ‘Prevalence and Determinants of Depressive and Anxiety Symptoms among Transgender People: Results of a Survey’, Healthcare (Basel, Switzerland), 11(5), available: https://doi.org/10.3390/healthcare11050705
Human Rights Watch (2010) ‘Iran: Discrimination and Violence Against Sexual Minorities: Laws, Policies Put Already Vulnerable People at Even Greater Risk’, 15 December. available: https://www.hrw.org/news/2010/12/15/iran-discrimination-and-violence-against-sexual-minorities
Jamali, S., Ghanbari, H. and Talebian Sharif, J. (2022) ‘A comparative evaluation of mental health, depression and post-operative role adaptation in Iranian transgender people living in Iran and Germany’, Journal of Principles of Mental Health, 24(1), 47–53, available: https://jfmh.mums.ac.ir/article_19542.html
Javaheri, F. (2010) ‘A Study of Transsexuality in Iran’, Iranian Studies, 43(3), 365–377. available: https://doi.org/10.1080/00210861003693893
Khorashad, B.S., Talaei, A., Aghili, Z. and Arabi, A. (2021) ‘Psychiatric morbidity among adult transgender people in Iran’, Journal of Psychiatric Research, 142, 33–39. available: https://doi.org/10.1016/j.jpsychires.2021.07.035
Feinberg, L. (1992) Transgender Liberation: A Movement Whose Time Has Come. New York: World View Forum.
Mazaheri Meybodi, A., Hajebi, A. and Ghanbari Jolfaei, A. (2014) ‘Psychiatric Axis I Comorbidities among Patients with Gender Dysphoria’, Psychiatry Journal, 971814. available: https://doi.org/10.1155/2014/971814
Meybodi, A.M., Hajebi, A. and Jolfaei, A.G. (2014) ‘The frequency of personality disorders in patients with gender identity disorder’, Medical Journal of the Islamic Republic of Iran, 28, 90.
Miller, L.R. and Grollman, E.A. (2015) ‘The Social Costs of Gender Nonconformity for Transgender Adults: Implications for Discrimination and Health’, Sociological Forum, 30(3), 809–831, available: https://doi.org/10.1111/socf.12193
Mohammadi, F., Masoum i, S.Z., Tehranineshat, B., Oshvandi, K. and Bijani, M. (2023) ‘Young transgender individuals' lived experiences of facing life's challenges: A qualitative study in Iran’, Frontiers in Public Health, 11, 1134237, available: https://doi.org/10.3389/fpubh.2023.1134237
Moradi, G., Riyahifar, S., Dehghanbanadaki, H., Bahrami, P., Zakaryaei, F., Sheibani, S., . . . Moradi, Y. (2023) ‘Prevalence of Mental Disorders and Their Risk Factors Among Iranian Transgender Population: a National Study’, Trends in Psychology. Advance online publication. available: https://doi.org/10.1007/s43076-023-00344-1
Nematollahi, A., Gharibzadeh, S. and Farnam, F. (2020) ‘Quality of Life and Mental Health in Iranian Transgender Women: Socio-Demographic Differences’, available: https://doi.org/10.21203/rs.3.rs-120558/v1
Pinna, F., Paribello, P., Somaini, G., Corona, A., Ventriglio, A., Corrias, C., . . . Carpiniello, B. (2022) ‘Mental health in transgender individuals: A systematic review’, International Review of Psychiatry, 34(3–4), 292–359, available: https://doi.org/10.1080/09540261.2022.2093629
Reisner, S.L., Vetters, R., Leclerc, M., Zaslow, S., Wolfrum, S., Shumer, D. and Mimiaga, M.J. (2015) ‘Mental health of transgender youth in care at an adolescent urban community health center: A matched retrospective cohort study’, The Journal of Adolescent Health: Official Publication of the Society for Adolescent Medicine, 56(3), 274–279, available: https://doi.org/10.1016/j.jadohealth.2014.10.264
Hill, R. (2007) A Social History of Heterosexual Transvestism in Cold War America (PhD Dissertation). University of Michigan at Ann Arbor, Michigan, United States.
Shirdel-Havar, E., Steensma, T.D., Cohen-Kettenis, P.T. and Kreukels, B.P.C. (2019) ‘Psychological symptoms and body image in individuals with gender dysphoria: A comparison between Iranian and Dutch clinics’, The International Journal of Transgenderism, 20(1), 108–117, available: https://doi.org/10.1080/15532739.2018.1444529
Shirdel-Havar, E., Yasrebi, K., Hassanzadeh, R., Moshkani, M. and Kaboosi, A. (2015) ‘Personality Disorders and Psychiatric Comorbidity among Persons with Gender Identity Disorder’, 3(Special Issue). Available at: https://psycnet.apa.org/record/2015-47418-017
Statistical Center of Iran (2017) Iran statistical year book 2016–2017, available: https://www.amar.org.ir/en/Statistics-by-Topic/Environment-and-multi-domain-statistics/Yearbooks-and-similar-compendia/Yearbook
Strauss, P., Cook, A., Winter, S., Watson, V., Wright Toussaint, D. and Lin, A. (2020) ‘Associations between negative life experiences and the mental health of trans and gender diverse young people in Australia: Findings from Trans Pathways’, Psychological Medicine, 50(5), 808–817, available: https://doi.org/10.1017/S0033291719000643
Stryker, S. (2008) ‘Transgender History, Homonormativity, and Disciplinarity’, 100(100), 145–157, available: https://doi.org/10.1215/01636545-2007-026
Talaei, A., Hedjazi, A., Badieyan Moosavi, N., Dadgarmoghaddam, M., Lotfinejad, N. and Khorashad, B.S. (2022) ‘The Epidemiology of Gender Dysphoria in Iran: The First Nationwide Study’, Archives of Sexual Behavior, 51(4), 1881–1889, available: https://doi.org/10.1007/s10508-021-02250-y
U.S. Institute of Peace (2024) ‘U.S. Report: LGBTQI+ Persecution in Iran’, 25 April, available: https://iranprimer.usip.org/index.php/blog/2024/apr/25/us-report-lgbtqi-persecution-iran
Wells, G.A., Shea, B., O’Connell, D., Peterson, J., Welch, V., Losos, M. and Tugwell, P. (2000) ‘The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses’, available: https://scholar.archive.org/work/zuw33wskgzf4bceqgi7opslsre/access/wayback/www3.med.unipmn.it/dispense_ebm/2009-2010/Corso Perfezionamento EBM_Faggiano/NOS_oxford.pdf