Author: Neil Majithia
Institution: Virginia Commonwealth University
Date: May 2009
When T.S. Eliot wrote the opening to The Waste Land, his primary intention was to capture the disillusionment of the post-World War I generation. For seasonal-allergy sufferers, however, a line such as "April is the cruellest month." must take on a dual meaning. Indeed, sometimes the most annoying symptoms are also the most harrowing, so for those 40 million Americans who bear runny noses and watery eyes through the spring and into the summer, there might as well be a war going on in the cellular trenches of their bodies.
This war is particularly intense for the estimated 26 million Americans experiencing chronic seasonal allergies, whose symptoms tend to be elevated and recurrent. For those with asthma and other severe conditions, allergies can jump the boundary from annoying to life-threatening in a frightening way.
Allergies affect a diverse population of individuals in an equally diverse manner. A study of the physiological phenomena responsible for seasonal allergies, as well as some of the medications (both out on the market and in development) used for treatment might help us better understand a large segment of our society. It will also help us see why allergies are such a hot topic in biomedical research, with a significant amount of NIH funding directed towards producing more effective treatments.
First of All, What Are Allergies?
While these may flowers look innocent, they can be an allergy-sufferers worst nightmare. Image courtesy of Extra Passive
In its physiological context, "allergy" refers to the body's hypersensitivity to certain environmental conditions. It is an exaggerated response of the immune system to substances that cause no harm in most individuals. Seasonal allergies describe a particular class of hypersensitivities based on seasonal conditions, particularly those of the spring and summer months when flowers are blooming and pollen spreads through the air.
Since allergies represent such a widespread occurrence of physiological malfunction, it is reasonable to wonder "why didn't evolution take care of that?" After all, it can hardly be a beneficial adaptation for people to be sneezing all throughout the months of April and May. Or can it? At least some scientists believe seasonal allergies are the result of an effective immunological adaptation that occurred thousands of years ago. You might say the road to runny noses was paved with good intentions.
In order to protect the body against the parasites and worms of those days, evolution came up with an antibody called immunoglobulin E (IgE) that is secreted into the intestines and lungs. While IgE was effective against ancient threats, many of the ancient threats are no longer around in today's environment so IgE lurks the bloodstream, looking to pick fights with other foreign substances entering the body. IgE fights dirty, and from a biochemical perspective, the cascade of chemical soldiers it calls into the fray is fascinating, so let's take a closer look at some of the players involved in this exaggerated immune response.
The Mechanism of False Alarm
When a person prone to allergies is exposed to an allergen (ragweed pollen, for example) for the first time, a type of immune cell called the plasma B-cell is stimulated to create a large amount of antibodies (in this case the antibody is IgE, and it serves more as an identification card than a molecule of direct defense). When the individual is exposed to that same allergen for a second time, IgE identifies the foreign substance, activates storage tank molecules called basophils and mast cells, and stimulates the release of additional defensive chemicals.
Among the chemicals released are histamine, heparin, and other factors that promote an extreme inflammatory response, characterized by local blood vessel dilation, cytokine release, and recruitment of leukocytes. While the inflammatory response is an important defense mechanism used to defend the body in the event of injury, in this case the body is defending itself against a harmless substance, so this "false alarm" causes irritation at the site of occurrence. Because mast cells are found in large quantities along the linings of the lung and nasal tract, the irritation often manifests itself in runny noses, dry coughing, or any of the symptoms commonly associated with seasonal allergies.
Overview of allergic response Image courtesy of Immune Central
Symptoms and Treatments
Seasonal allergies commonly make their presence felt through a condition called allergic rhinitis, or "hay fever." Despite its name, hay fever does not result in an actual fever. Instead, it is similar to the common cold, with certain differences that can make it a more uncomfortable experience. For example, while a cold may last for a week or two, hay fever can stretch out for several months with little improvement in condition. Colds generally produce nasal discharge that is thick and yellow, whereas hay fever produces a nasal discharge that is clear, thin, and "runny." These symptoms might also be accompanied by general itchiness of the eyes or skin.
Oftentimes an individual might have a hunch that he or she is suffering from seasonal allergies, but it can be a challenge to identify the causative allergen. From a brief medical history, a doctor will put together a list of suspected allergens, and to confirm the diagnosis, or to crack particularly puzzling cases, she will carry out a skin test. Several punctures are made (generally on the patient's back or forearm), each containing trace amounts of a suspected allergen. A positive result is indicated by a "wheal and flare," a hive-like red bump at the site of puncture.
Schematic diagram of allergy skin test Image courtesy of Your Total Health
There is no known cure for allergies, but there are treatments that can make the symptoms less severe. The most obvious way of preventing symptoms is to avoid those allergens that cause them. Unfortunately this can be rather inconvenient for those who would like to enjoy the great outdoors during the beautiful spring and summer months. All sorts of allergens are floating around in the air, so life for an allergy sufferer can be anything from annoying to downright miserable. Fortunately there are a wide variety of medications available to ease the agony.
The most common type of allergy medication is called an antihistamine. Thinking back to histamine's function in the mechanism of allergies, we saw how the molecule was involved in the inflammatory response. It specifically initiates vasodilation, allowing increased blood flow to a particular region in the body (thus increasing the level of immunological factors at the site of invasion). It is this cascade of events that results in the symptoms of seasonal allergies. Blocking histamine, then, would prevent this from occurring, so while it would not cure the allergy (IgE would still erroneously recognize its specific allergen as harmful), it would certainly alleviate some of the misery caused by the allergy.
Antihistamines do not come without side-effects, however. Many antihistamines cause drowsiness, making them difficult to take in the middle of the day. There are certain "non-sedating" antihistamines available on the market that claim to provide all the benefits of allergy alleviation without the potential drowsiness. Dr. Peter Honig, a medical officer at the FDA suggests the term non-sedating is a misnomer, since all anti-histamines cause drowsiness,it is just a matter of how sedating each product is. Benadryl, for example, is heavily sedating, whereas Allegra and Claritin are less so.
Alternative Solutions
For some people, typical allergy medications simply are not enough. There is still hope for them though, and it comes in the form of a process called immunotherapy. The aim of immunotherapy is to desensitize the immune system to allergens by administering a series of shots over the period of several years. These shots contain trace amounts of the allergen and after a while the immune system "learns" that it is harmless.
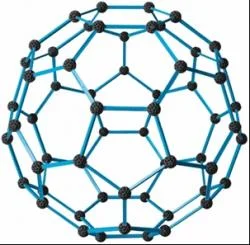
An alternative strategy is to block the harmful effects of the immune system. Buckminsterfullerenes, or "buckyballs," are a hot topic in all sorts of research circles, including those working on allergy relief. An article written by JYI's own Jeremy Fagan covers the breakthrough at a Virginia Commonwealth University lab working to characterize the buckyball's therapeutic capabilities (to read Jeremy's article click here: http://www.jyi.org/news/nb.php?id=1106). Dr. Chris Kepley's research team discovered that the 60-carbon cage structure of a buckyball was able to prevent the activation of IgE, and thus prevent the release of inflammatory molecules. What's more, the buckyballs did not cause any sort of toxicity in the cell's internal environment, indicating buckyballs might, with the addition of certain functional groups, eventually serve as powerful, precise allergy inhibitors.
Schematic picture of a buckyball, distinguished by its 60-carbon, soccer ball-like appearance. Image courtesy of Ozpod
One of the fascinating aspects of allergy research, though, is the varied approach researchers take to preventing inflammatory response. A team of researchers working at Beth Israel Deaconess Medical Center (BIDMC) has taken a more genetic approach, focusing on knocking out calcium channels on mast cells, which are necessary for the release of inflammatory factors. The group identified a specific gene (CRACM1) as being responsible for the coding of this calcium channel, and by inhibiting its expression in mice, noticed a significant improvement.
Monica Vig, lead researcher of the BIDMC team, reported, "With the identification of this long-elusive gene, we were able to create a knockout mouse that lacked CRACM1, and [as predicted] these animals proved to be resistant to various stimuli that usually cause severe allergic reactions."
Jean-Pierre Kinet, professor of Pathology at Harvard Medical School, and member of the project added, "These findings provide the genetic demonstration that CRAC channels are essential in mast-cell activation.This provides the proof of concept that an inhibitor of the CRAC channel should be able to impact mast-cell related diseases, including asthma and allergic diseases."
Alternative Solutions
The allergic response is just one example of how the immune system can simultaneously be a blessing and a curse. Our immune cells are absolutely essential to our survival because they have the ability to identify and eliminate foreign pathogens; however, if something goes wrong, these same cells might overreact and, in some particularly devastating cases, attack the body's friendly cells with a devastating potency. Fortunately seasonal allergies can be controlled, and with even more promising treatments on the horizon, science is doing what it can to make April as pleasant as possible.
References
1) Janeway, Charles; Paul Travers, Mark Walport, and Mark Shlomchik. Immunobiology (Fifth Edition). New York and London: Garland Science, 2001.
2) Croner S. "Prediction and detection of allergy development: influence of genetic and environmental factors". J. Pediatr. 1992, 121.
3) Williams, Rebecca D. "Watery Eyes? Runny Nose? Time to Spring into Action Against Seasonal Allergies." FDA Consumer. March-April 1998, 15-16.
Written by Neil Majithia
Reviewed by Pooja Ghatalia
Published by Pooja Ghatalia