Author: Kushner Emily
Institution: Biological life sciences
Date: September 2005
During the sultry summer months in quiet towns across the United States, mothers are making their children wait to go outside and play. Why is the fun being taken out of these precious last hours of daylight? A villain lurks outside, more evil, more aggravating, and the cause of more itching than you can imagine , the mosquito. Mothers in the United States have long been used to battling the mosquito's wrath during the summer months by insisting , amidst all the moaning and complaining , that their children be thoroughly sprayed with mosquito repellent before they can play outside after dinner. But the goal used to be simply to avoid the itch that resulted from the mosquitoes' bites. Why is this practice now becoming more and more prevalent all over the country? In 2002, the United States, for the first time ever, had the highest number of reported West Nile Virus infections in the world. About 3,600 Americans fell victim to the potentially fatal mosquito-borne virus over the last year. However, with increased awareness regarding the disease, its history, symptoms, and means of transmission, more people will have the know-how to ward off infection in 2003 and beyond.
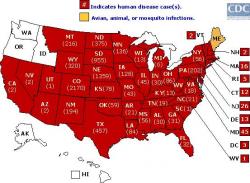
Figure 1. Reported cases of West Nile Virus in the United Sates in 2003 (data current as of October 22, 2003). Numbers in parentheses correspond to the number of human cases per state. Source: Centers for Disease Control and Prevention.
West Nile Virus was first isolated in Uganda in 1937 and is a member of a classification of viruses known as the flaviviruses. This simply means that it is carried by insects and causes disease in humans and other animals. Commonly found in Africa, West and Central Asia, and the Middle East, the virus was first identified in the United States in 1999 as the cause of severe and fatal human illness in metropolitan New York City. The Centers for Disease Control and Prevention (CDC) became aware of the presence of West Nile in America when birds began inexplicably dying in large numbers near the Bronx Zoo in New York. It is not know how the virus was first introduced into the United States, but since its initial appearance, it has spread rapidly and was found throughout the eastern half of the country by the summer of 2001. Many theories immediately surfaced about how the disease could have made the journey across the Atlantic but a definite source has not been identified. It is possible that an animal carried the disease overseas, or that a stowaway insect decided to wreak havoc on the Bronx bird population. Although the vast majority of infections have been identified in birds, West Nile Virus has been shown to infect a range of animals including horses, cats, bats, squirrels, and domesticated rabbits.
Disease Background
West Nile Virus is a progressive disease with two viremias. A viremia is a medical term meaning that a virus is present in the bloodstream of an animal. The first, less severe viremia is West Nile Fever. The second is West Nile Encephalitis. Of those infected with West Nile Virus, only 20% develop West Nile Fever, and less than 1% of that small group will develop West Nile Encephalitis. The CDC reports that of the roughly 3,600 patients diagnosed with West Nile Fever in 2002, 232 died due to their illnesses, which is 6% of the total number infected. This may seem like a lot, but it is still relatively low compared to other infectious diseases such as yellow fever, another mosquito-borne virus, which has a 15% mortality rate (30,000 deaths per year out of 200,000 reported cases).
"It is possible to develop West Nile Fever and not even know you have it that's how mild the illness can be," says Dr. Geraldine Luginbuhl, a professor of Medical Microbiology at North Carolina State University. The symptoms include fever, headache, muscle ache, swollen lymph glands, and occasionally a rash. Therefore, the disease often goes undiagnosed because these symptoms are similar to those of a cold or the flu. Luginbuhl also confirms that there are no long-term effects of West Nile Fever, and that symptoms tend to only last a few days.
West Nile Encephalitis is a much more severe infection and sometimes causes extreme damage to the human body. Symptoms include a stiff neck, stupor, disorientation, coma, tremors, convulsions, and even paralysis. Although symptoms will not last forever (they usually last for about three weeks), the effects of the illness are potentially permanent.
Fortunately, in most cases West Nile runs its course and the troubles are over; no chronic infections are associated with West Nile Virus. As with other infections, the B lymphocytes produced by the body's immune system are kept forever and make it easier for the body to respond to the infection if exposed a second time.
Diagnostic practices are being improved quickly by the medical world to combat the increased number of West Nile Virus cases. One major breakthrough came in May 2002, when the National Institute for Neurological Disorders and Stroke (NINDS) announced a more efficient way to diagnose West Nile Virus in The Lancet, a British medical journal similar in content and prestige to The New England Journal of Medicine. The NINDS technique, which relies on a DNA quantification procedure called real-time PCR, is capable of detecting minute amounts of West Nile and can do so in a mere 5 hours. The traditional method of detection can take up to 5 days.
Treatment of West Nile infections, unfortunately, has yet to allow anyone bragging rights. "There are no specific antibiotics or treatment drugs to ward off an infection," laments Dr. Luginbuhl. Patients with West Nile Fever are generally prescribed over-the-counter drugs such as acetaminophen to treat their symptoms because there is not yet a drug to fight the actual virus. In the case of West Nile Encephalitis, hospitalization is often required since the disease is of greater severity.
Modes of Infection
The principle transmission cycle of West Nile Virus is from insects to birds or animals. Mosquitoes become infected with West Nile when they feed on the blood of a bird carrying the virus. The insect then carries the virus around with them while the virus matures and travels through the body to the salivary glands. After about 12 days of incubation with the virus, the insect can then pass the infection on to another animal or human, also during blood feeding. The mosquito injects the virus contained in its saliva into the bird or animal, where it replicates and causes illness. Although humans and other mammals may develop an infection in response to West Nile, humans do not produce enough of the virus to transmit it to others or to infect mosquitoes.
The virus can also be transmitted in other ways. In some cases, West Nile has reportedly been the cause of infection in patients receiving infected blood transfusions and organ donations. Public health agencies are encouraging all those who want to donate blood to be tested if they are experiencing symptoms similar to those described above. Blood that has caused infections is immediately pulled out of the blood bank and disposed of to prevent the risk of further infection The Secretary of the Maryland State Health Department, Dr. Georges Benjamin, wants people to remember that contraction of the West Nile virus cannot occur from donating blood or organs. "We want people to continue giving the gift of life whether it is blood or an organ," said Benjamin in a press conference concerning the virus. Blood banks are always in need of donations, and after the infection is gone, it is safe to begin donating once again. The Food and Drug Administration also reminds potential donors that "donating blood carries no risk of acquiring West Nile Virus." And says that "for those who need blood transfusions, the benefits outweigh the risk of acquiring the virus."
A Warning to Pregnant Mothers
As with most viruses and illnesses, pregnant mothers should take extra precautions to prevent themselves from becoming infected with West Nile. Recently, active West Nile Virus was detected in infants who breastfed from infected mothers. On December 19, 2002, the first case of a child being infected during pregnancy was reported in Onondaga County, NY. The infant was born with defects including loss of brain mass. The CDC said it is not yet clear if the infection caused the abnormalities, but both the CDC and the county health official involved said people ought to be aware of the possibility that unborn children can contract the virus.
Steps to Take to Ensure Safety
Unfortunately there is no definite way to protect oneself from a West Nile infection since there is no vaccine, although research is being done to develop one. The CDC reports that your best bet for prevention is to protect yourself from insect bites, since this is how the virus is usually transmitted. It recommends limiting outdoor activity during the warmer months around dusk, because this is when mosquitoes are most prevalent. It also suggests that you wear long pants and shirts and spray your clothing with insect repellent before leaving your house. The most effective repellents contain up to 50% DEET (any higher does not offer any extra protection) for adults and around 10% DEET for children up to age 12.
Figure 2. Some steps to prevent the spread of West Nile Virus. From left to right: remove standing water from outdoor containers, use mosquito repellent containing DEET, wear long shirts and spray clothing with insect repellent to deter mosquitoes. Source: Centers for Disease Control and Prevention.
Also, avoid inadvertently breeding mosquitoes in your yard. Make sure that standing water is not allowed to sit in small pools, flowerpots, or watering cans since these are prime locations for mosquito havens. On a community level, the CDC urges you to keep your eyes open for dead or dying birds and report them by contacting your local health department.
West Nile Virus has proven itself to be no laughing matter. Luckily, there are many ways to help combat the spread of the virus. Knowing about the enemy is always the first step in fighting an opponent. Be aware of the potential risks in your area and keep your family safe by taking the necessary precautions , children everywhere will thank you for their extra playtime.
Websites Related to this Topic
CDC West Nile Homepage WRAL News - Health and West Nile Virus West Nile Distribution Maps West Nile Fever
Suggested Reading
Briese, T., et al. Detection of West Nile Virus sequences in cerebrospinal fluid. The Lancet. 355: 1614-5 (2000)
Fine, A., et al. Testing for West Nile Virus. The Lancet. 356:1110-1 (2000)
Han, L.L., et al. Risk Factors for West Nile Virus Infection and Meningoencephalitis, Romania, 1996. Journal of Infectious Diseases. 179:230-3 (1999)
Stephenson, J. Nailing West Nile Virus. Journal of the American Medical Association. 283:3060 (2000)